
While many people associate post-traumatic stress disorder (PTSD) with military combat, the truth is this condition can affect anyone. In fact, the U.S. Department of Veterans Affairs has noted that 13 percent of women and 25 percent of men report car crashes as being traumatic, life-changing events. As such, vehicle accidents can and do lead to both acute and chronic PTSD for many survivors.
Even minor crashes can have long-term psychological effects on someone who has been in an accident. After all, the overall intensity and emotions related to any highway collision can stir feelings of confusion, doubt, worry, anxiety, depression, flashbacks and nightmares.
People who have experienced a single or multiple vehicle crash may want to chart their mental health carefully post-accident. Otherwise, they might unnecessarily pay a high price due to undiagnosed, untreated PTSD.
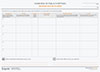
Sample accident journal/diary to help you document the effect on your daily life
Download in PDF format
Linking motor vehicle accidents to PTSD
Not every person involved in a car accident gets PTSD, but at least nine percent and up to around 60 percent are likely to experience it. These figures shed light not only on how widespread crash-related PTSD can be, but how it can affect both a survivor and those around them.
For instance, after a car accident, a victim may exhibit signs of hesitation upon getting into another vehicle. Without intervention such as working with a mental health provider, the individual may find traveling to work difficult, if not impossible.
Thus, lingering PTSD symptoms might lead to increasing stress and negative personal and business relationships. In a situation such as this, the victim could eventually lose their job, alienate loved ones, or sink into a depressive state.
Another example of the way PTSD can affect a family is when a victim starts “acting out” with abusive behavior toward themselves or others. Self-harm and lashing out can cost the victim a safe home life; it can even lead to imprisonment if they cannot control outbursts. In children with PTSD, schoolwork, peer relationships, and reputation may be sacrificed if they don’t receive intervention.
Some people are more prone to PTSD than most, such as those who have been in previous accidents, were seriously hurt (or watched someone else get injured or die) or already have risk factors for PTSD like having depression. Plus, PTSD can take many weeks or even months to present itself fully, making documentation of key importance.
At the end of the day, the only way to know whether a child or adult who has been in a vehicle crash has PTSD is via a comprehensive healthcare evaluation. Typically, providers look for recurring symptoms to determine whether PTSD is indeed at play.
Moving forward after crash-related PTSD
After diagnosis of PTSD, car accident victims can expect to spend time in therapy learning the best ways to cope with their feelings. By acknowledging the intense, overwhelming event, they can work through responses to minimize the effects of the condition.
Over time, PTSD can be managed and overcome with hard work. However, it can be costly for those without major medical coverage or a way to pay for therapy sessions or cover mounting bills due to PTSD-related job loss. If you or a loved one experience documented, diagnosed PTSD after being in an accident that wasn’t your fault, consider pursuing legal means to attempt to receive compensation from the at-fault party.
Clearly, PTSD is a problem among those who have been through auto accidents, even so-called “fender benders.” Like all physical and mental outcomes post-crash, any PTSD signs should be addressed immediately. In this way, PTSD sufferers can get the help they need and avoid months or years of setbacks, expenses, and further emotional trauma.
 Steven G. Wigrizeris an experienced trial attorney who has been repeatedly recognized as one of the best in his field. He concentrates his Philadelphia, Pennsylvania practice in complex civil litigation including medical malpractice, products liability, pharmaceutical liability, car/truck accidents, maritime disasters, workplace accidents and class actions.
Steven G. Wigrizeris an experienced trial attorney who has been repeatedly recognized as one of the best in his field. He concentrates his Philadelphia, Pennsylvania practice in complex civil litigation including medical malpractice, products liability, pharmaceutical liability, car/truck accidents, maritime disasters, workplace accidents and class actions.