
When the wrong prescriptions cause personal injuries
Pharmacists give medical advice, know how medications interact, and offer help when we’re sick. If we are ingesting pills that are supposed to do something, then by God, we want to make sure they’re the right ones to take.
But what happens when the pharmacy makes an error? How often does it happen?
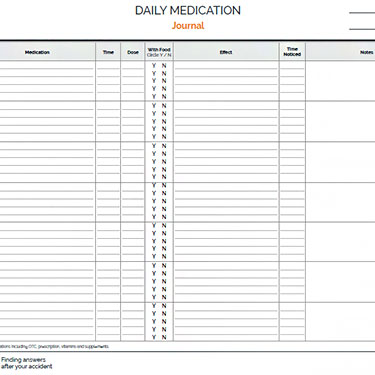 Medication Log Sheet
Medication Log Sheet
Printable daily medication log template helps you track your medicines and side effects
Download in PDF format![]()
Pharmacists take their time in making sure that a prescription is correct, and they have many safeguards before it leaves the premises.
Additionally, there are labels on the bottle and descriptions of what the pill should look like to the consumer. The drugs are also accompanied by literature explaining what the medication is, what it does and what the potential side effects are.
Tweet this
Sometimes, somehow, the incorrect pill can slip by those safeguards, and the user can end up with the wrong prescription or the wrong dosage.
How does this happen?
How do pharmacy mistakes happen?
Pharmacists are humans before anything else. As such, there is the capacity for human error.
The impending march of technology hasn’t relegated pharmacists to the unemployment line yet, but that means the human brain – fickle as it is – can’t interfere with the process of filling a prescription.
 Post-Accident Journal Form
Post-Accident Journal Form
Sample accident journal/diary to help you document the effect on your daily life
Download in PDF format![]()
Here are some ways that this can happen:
- Understaffing: This is especially true of the chain pharmacies, like the ones you find in grocery stores or your “big box” competitor stores. Pharmacists usually have little control over scheduling and staffing there, so if a tech doesn’t show up that day, they are out of luck and have to scramble. This can mean the increasing likelihood of an error – or several.
- Exhaustion: If a pharmacy is understaffed, this might lead a pharmacist to volunteer to take extra hours. It’s one thing to volunteer because you want to make extra money, but what if your boss pressures you?
- Pressure to work too quickly: Many pharmacies have a limit on the number of scripts that pharmacists can write per day or per hour, but they might be ignored in the effort to keep up with the line snaking out the door.
- Upset: Fighting with a family member or staying up all night taking care of a sick child can put anyone, including a pharmacist, into a bad head space, which can lead to errors. They’re only human, after all.
- Misreading: Doctors have famously messy handwriting. If a pharmacist or tech misreads their handwriting, this can result in an incorrect prescription. While this isn’t too common now with electronic coding and prescriptions ordered by computer (which can also present problems if the incorrect code is entered by the physician), if a patient presents a handwritten prescription, this can still occur.
- Names that sound alike: Many drugs have names that just sound too similar. Try some of these on for size: Amicar and Omacor. Altocor and Advicor. Enjuvia and Januvia. Duloxetine and Fluoxetine. Fluoxetine and Paroxetine. Guanfacine and Guaifenesin. Confused yet?
- The next drug on the shelf: Sometimes the pharmacist accidentally grabbed the medication next to the one they meant to pull, simply because he or she was moving too fast. Have you seen those shelves?

- Patient misidentification: It’s actually a drug meant for someone else. This is rare because of lockout procedures (birthdates, addresses and the like intended to keep you from receiving the incorrect medication), but it still does happen.
- Declined counseling: Usually when a medication is dispensed from the pharmacist to the patient, the pharmacist will ask if the patient wants to discuss the uses and side effects. The patient can say yes or decline the counseling. Many safety councils say that requiring counseling would help reduce pharmacy error by a significant amount, because if a patient were expecting, for instance, pain medication, and instead received a blood thinner, he or she would be alerted during counseling that the drug was not what was expected.
It is an entirely subjective examination as to what the situation was surrounding the error and why the pharmacist made the mistake.
That is why just denouncing the pharmacist isn’t always the best solution. It is not always simple negligence or even reckless disregard; there is always a more complicated story that must be explained and investigated to keep that mistake from happening again.
When it comes to prescription drugs, Big Pharma often plays roulette with consumers' health. Drug companies have had to pay billions in settlement and judgments for violating federal laws, withholding safety information, fraud, and other illegal activities. Find out more
The pharmacists’ duty of care
Pharmacy malpractice is a type of personal injury law that comes under the theory of negligence. This means that the following must be true in order for the victim to prevail:
- The pharmacist owed a duty of care to the patient;
- The pharmacist breached that duty of care;
- The breach was the proximate (legal) cause of the patient’s harm; and
- The breach caused damages.
A relationship is established between a pharmacist and patient who fills a prescription at that pharmacy.
This means that the pharmacist has a duty of care toward that patient, and that duty also extends to the establishment in which that pharmacist works. Considering that the pharmacist has the degree and is licensed by the state, he or she is held to a higher standard of care. (However, the burden falls upon the plaintiff to show that the defendant breached that higher standard of care in a medical malpractice lawsuit.)
The important piece – the most difficult, to be sure – is showing proximate cause. This is the legal cause, which in a negligence cause means that the victim’s injuries were foreseeable. If the plaintiff’s injuries were not foreseeable, then negligence cannot be established.
The plaintiff must show that the pharmacist’s negligence in prescribing the incorrect medication is actually what caused his or her injuries. Some states use different tests for determining proximate cause, such as the but for test or the substantial factor test.
The “But For” test
The But For test states exactly that: But for the defendant’s conduct, the plaintiff’s injuries would not have happened. So, in this case, but for the pharmacist’s conduct (prescribing an incorrect medication), the patient would not have been injured.
The Substantial Factor test
Here, courts consider factors in determining whether the defendant’s actions (here, a pharmacist prescribing an incorrect medication) were a substantial factor in causing the plaintiff’s injuries.
What damages are available in a pharmacy malpractice case?
Most likely, damages will include compensation for medical expenses, disability, pain and suffering, loss of earnings, and perhaps emotional distress.
 Damages/Expenses Worksheet
Damages/Expenses Worksheet
Damages worksheet to track expenses for your injury claim (medical treatment, property damage, lost wages, prescriptions)
Download in PDF format![]()
The court might also consider other compensation as well, depending on how severe the patient’s injuries were and how bad of a medication mix-up it was.
The pharmacy or hospital for which the pharmacist worked will also be liable under the theory of respondeat superior, or “let the employer answer.”
This means that the employer is responsible for the acts of the employee during company hours. They will argue this as hard as possible, because they have deep pockets and can afford to do so. However, if that pharmacist was filling prescriptions during regular business hours, they will most likely lose.
 Personal Injury Attorney Interview Sheet
Personal Injury Attorney Interview Sheet
Worksheet with questions to ask a personal injury attorney to help determine if he or she will be a good fit for your case
Download in PDF format![]()
Additionally, if the pharmacy error was truly unforgiveable, the court might apply punitive damages to the case. These are damages meant to punish, and in applicable, they would be slapped against the pharmacist, pharmacy, hospital or other entity that could potentially be held responsible for the error.
Finding an attorney who is proficient in pharmaceutical errors and medical malpractice can be difficult. If you need one, consider speaking with someone in the Enjuris law firm directory – they will be able to help.
See our guide Choosing a personal injury attorney.

